How the Pomona Valley case signals a shift for privacy breach in healthcare
On November 6, 2025, The HIPAA Journal reported that Pomona Valley Hospital Medical Center (PVHMC) agreed to pay $600,000 to settle a class action lawsuit over its use of Meta Pixel and similar website-tracking technologies.
The case, Warren v. Pomona Valley Hospital Medical Center, centered on how these tools may have unintentionally transmitted user identifiers and patient information to third parties such as Meta (Facebook). This case highlights a growing reality across healthcare: not all data risks come from hackers. Some emerge quietly from well-intentioned tools never designed with patient privacy in mind.
A privacy challenge for healthcare websites tracking tools
No ransomware. No malicious intrusion. Yet, as with many organizations navigating digital care, sensitive data may have moved beyond expected boundaries.
Between 2019 and 2022, website tracking technologies embedded on PVHMC’s patient portal collected behavioral and technical data. In certain cases, that information could be linked to individuals, creating a potential privacy exposure that regulators and courts now interpret as a breach of trust, if not security.
The $600,000 settlement will provide payments to California residents who accessed the hospital’s patient portal during that period. But the implications extend well beyond a single institution. This reflects a broader challenge many healthcare providers face – managing the invisible flow of data between marketing tools, analytics platforms, and third-party networks.
It’s also a reminder that risks don’t always stem from new surfaces. Technologies implemented years ago under different privacy expectations can resurface today as compliance challenges, highlighting the need for continuous vigilance.
The expanding definition of “HIPAA data breach”
We’re witnessing a shift from data loss to data exposure as the new measure of accountability.
Healthcare organizations have long focused on keeping data safe from external attackers. But today, regulators and courts are asking a more nuanced question:
“Who else is receiving data from your systems without the patient’s consent?”
That includes marketing trackers, analytics pixels, social media plug-ins, and chatbots that capture digital interactions on patient-facing websites.
The Pomona Valley case joins a growing number of legal actions where pixels and cookies are treated as potential vectors for unauthorized data sharing, especially under HIPAA, the CCPA, and emerging federal privacy frameworks. Even anonymized or hashed data may qualify as protected if re-identification is possible.
For healthcare marketers, this means digital engagement and privacy compliance can no longer exist in separate silos. These functions must align operationally, sharing the same data visibility, compliance goals, and understanding of patient trust.
Why it happened and why it keeps happening
Digital transformation has been instrumental in improving patient experience. But as healthcare organizations expand their digital presence, many lack full visibility into what their websites share with third-party domains, especially as those integrations evolve over time.
These invisible interactions represent client-side risk, where data exchanges occur within a user’s browser rather than an organization’s secure server environment. Traditional security tools rarely detect these risks.
Even well-encrypted systems and consent mechanisms can’t fully prevent exposure when tracking tools capture behavioral data that can be linked to health information. If user activity can be connected to patient identity, compliance obligations apply.
And because these risks can remain dormant for years, visibility into historical configurations is just as critical as monitoring new ones.
How to prevent Meta pixel HIPAA violations

The Pomona Valley incident is a growing challenge shared across the healthcare industry. This case illustrates that even well-intentioned digital strategies can create unseen data pathways. A more coordinated approach between compliance, IT, and marketing teams could help mitigate these risks. This approach includes:
- Pre-implementation data mapping: Identify which pixels or SDKs process user data and where that data flows.
- Consent and configuration controls: Ensure analytics tools don’t collect or transmit PHI or identifiable data.
- Cross-team collaboration: Conduct regular privacy impact assessments across compliance, IT, and marketing teams.
- Continuous client-side monitoring: Detect when scripts or pixels begin transmitting sensitive data in real time.
Each of these steps supports a larger mindset shift: data privacy isn’t a static policy but a continuous process of verification and shared accountability.
How AI can strengthen continuous monitoring
Artificial intelligence is becoming indispensable in managing today’s complex digital ecosystems. AI-driven monitoring can analyze web behaviors in real time, identifying which scripts are active, where data travels, and whether new or unauthorized connections appear.
Instead of relying solely on periodic audits, organizations can maintain continuous visibility by detecting potential data exposures before they reach unauthorized recipients.
AI acts as a digital observer, recognizing anomalies faster than manual review ever could, and helping organizations stay alert to both emerging and legacy risks.
Five practices to protect patient privacy and digital trust
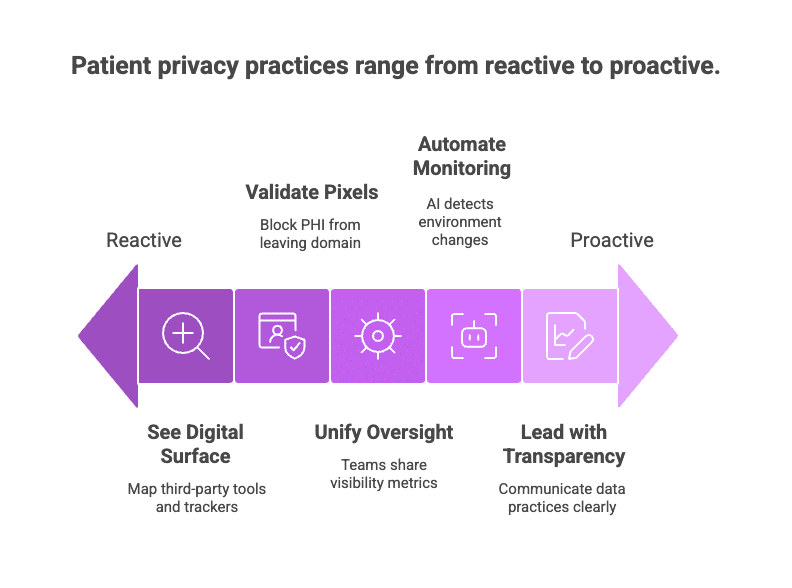
1. See your full digital surface.
Map every third-party tool, tag, and tracker that interacts with your website or application.
2. Validate your pixels.
Ensure marketing technologies are configured to block PHI or identifiable data from leaving your domain.
3. Unify your oversight.
Bring together the legal, compliance, marketing, and IT teams around shared visibility metrics.
4. Automate your monitoring.
Use AI or automated scanning tools to continuously detect and assess changes in your client-side environment.
5. Lead with transparency.
Communicate clearly with users about data collection practices. Trust grows in openness and accountability.
The bigger picture
The Pomona Valley case opens a conversation about what constitutes a “data breach” in a digital-first healthcare landscape.
Security is no longer confined to firewalls and encryption keys. It resides in the scripts that track engagement, the pixels that personalize content, and the APIs that power convenience. Each can quietly become a point of exposure if left unchecked. Having full visibility into what happens on your client side is how organizations can protect both data and trust, acknowledging that unseen data flows are the new frontier of risk in the ever-evolving digital healthcare landscape.





